Employee experience strategy for hospital networks in 2026
An employee experience strategy for hospital networks is a system-level approach to designing, managing, and measuring workforce experience across multiple care sites. It aligns clinical workflows, HR practices, and leadership governance along with the use of healthcare survey tools to ensure consistent, high-quality employee experience healthcare strategy across the network.
This guide is built on tested frameworks used by leading healthcare industry experts to design, scale, and govern multi-site healthcare employee experience with precision and accountability.
- An employee experience strategy for hospital networks is a system-level approach to designing how work is structured, delivered, and improved across multiple care sites.
- EX priorities differ: acute care requires speed, community hospitals need continuity, specialist centers require autonomy, and aged care demands emotional support.
- Governance should follow a hub-and-spoke model: the central team sets standards and measurement frameworks; individual sites customize design and respond to local feedback.
- Workforce experience must be measured at three levels, group, site, and department, to identify trends, variation, and root causes separately.
- CultureMonkey enables hospital networks to run this strategy with multi-channel surveys, role-based dashboards, and real-time cross-site EX analytics.
What is an employee experience strategy for hospital networks?

An employee experience strategy for hospital networks defines how work is designed, delivered, and improved across multiple care sites. It ensures employee experience healthcare is consistent across roles, departments, and the full care delivery lifecycle.
EX vs engagement healthcare: Employee experience covers the full arc of work, from recruitment to exit. Engagement measures how engaged and satisfied employees feel at a specific point in time, not how the system operates daily.
In the healthcare industry, this difference is critical. Engagement scores can remain stable while experience gaps across shifts, departments, and sites still drive workflow inefficiency, handoff breakdowns, and interdepartmental friction with employees struggling to find a work life balance, without peer support.
Why employee experience healthcare strategy fails in multi-site hospital networks
Employee experience healthcare strategy fails in multi-site hospital networks due to three predictable breakdowns: standardization, centralization, and poor measurement. These issues make multi-site healthcare employee experience and engaged employees inconsistent and lead to network EX failure.
1. Standardization ignores site realities
Uniform design in health systems overlooks how work differs across hospitals.
- Acute, community, and specialist sites operate with different workflows, staffing models, and employee health pressure levels.
- A single approach creates gaps between designed processes and actual daily operations.
2. Centralized decisions miss frontline context
Top-down strategies in health systems fail to reflect real operational conditions.
- Leadership defines experience without input from clinical and non-clinical staff.
- Teams stop responding or acting on feedback when local issues remain unresolved, hindering organizational values.
3. Measurement hides variation across sites
Aggregated data masks where experience actually breaks.
- Network-level scores of engagement metrics hide differences between departments, roles, and shifts.
- Leaders act on averages instead of identifying specific site-level breakdowns of engaged employees of healthcare organizations.
(Source: Press Ganey)
What framework do hospital networks use to design EX by site type?

Hospital networks use the Site-Type EX Matrix to define distinct experience priorities for each care site type. It maps four experience profiles: acute, community, specialist, and aged care, and specifies what must be designed differently in each environment.
Without this framework, networks default to uniform EX design that consistently underperforms in high-intensity or long-term care settings.
1. Acute care hospitals: Speed, coordination, and decision clarity
Design principle: Standardize escalation pathways before customizing communication tools.
- Focus on shift coordination, rapid communication, and clear escalation pathways to boost employee engagement.
- Reduce friction in handoffs, staffing decisions, and emergency workflows to improve employee satisfaction and improved patient care.
2. Community hospitals: Continuity, stability, and workload balance
Design principle: Prioritize schedule consistency above any other experience intervention.
- Focus on workload distribution, role clarity, and consistent scheduling to create a positive employee experience.
- Strengthen team cohesion and reduce fatigue from repetitive workload cycles to provide exceptional patient care.
3. Specialist centres: Expertise, autonomy, and precision
Design principle: Reduce administrative load first, autonomy is undermined by paperwork, not by management style.
- Focus on autonomy in decision-making and access to advanced tools with predictive analytics by the workforce management.
- Minimize administrative burden that disrupts clinical work and affects the employee's healthy work life balance by leveraging technology.
4. Aged care settings: Empathy, consistency, and emotional support
Design principle: Measure emotional fatigue separately from general workload, because they require different interventions.
- Create environments that focus on staffing consistency and relationship continuity for continuous improvement of the culture.
- Providing employees support systems for shift workers with emotional fatigue and caregiver stress is a major factor to improve overall employee satisfaction.
Organizations that prioritize recognition and support experience lower attrition rates, as employees are more likely to stay when they feel valued, leading to increased stability in staffing and a positive impact on patient care.
7 Employee Engagement Tips to Boost Your Practice’s Culture
How to build an employee journey map in healthcare across hospital networks?
To build an employee journey map healthcare across hospital networks, map the full clinical staff lifecycle in healthcare teams and define experience requirements at each stage. Each stage in the clinical staff lifecycle has different experience design requirements.
Treating these stages uniformly creates gaps in experience, especially across roles, shifts, and hospital types and gives increased job satisfaction. Recognizing team contributions increases employee connection to workplace culture significantly.
How does EX design differ for nurses versus physicians versus administrative staff?
EX design must be role-specific in hospital networks. Nurses, physicians, and administrative staff have different pressure points, retention drivers, and experience breakdown patterns, a single journey map applied across all three groups consistently misses the signals that precede role-specific attrition.
What governance model works for EX governance in multi-site hospital systems?

The hub-and-spoke model works best for EX governance multi-site hospital systems because it balances central standards with site-level flexibility. It sets central standards while enabling site-level customization within a hospital group people strategy.
Central hub: Define standards and guardrails
The central team defines what must remain consistent across the network in healthcare organizations.
- Set EX principles, measurement frameworks, and non-negotiable policies to create a motivated workforce.
- Standardize data models, survey methods, and reporting structures to see particularly those who are facing employee burnout before it affects operational efficiency, workforce stability and company culture.
Site spokes: Adapt to local realities
Individual healthcare organizations adjust experience design based on their context.
- Customize workflows, communication methods, and interventions at the site level to contribute to organizational success.
- Act on local employee feedback by using engagement strategies without waiting for central approvals.
Governance link: Connect decisions across levels
A structured link ensures coordination in healthcare organizations without slowing execution.
- Define clear decision rights and critical metrics between central and site teams and see who provides exceptional patient care.
- Review performance regularly to maintain consistency and flexibility to create a more resilient workforce and supportive culture without medical errors.
Without a hub-and-spoke governance structure, hospital network EX programs produce one of two failure modes: the central team enforces rules that ignore site-level operational reality, or individual sites build isolated programs that cannot be compared or improved at scale.
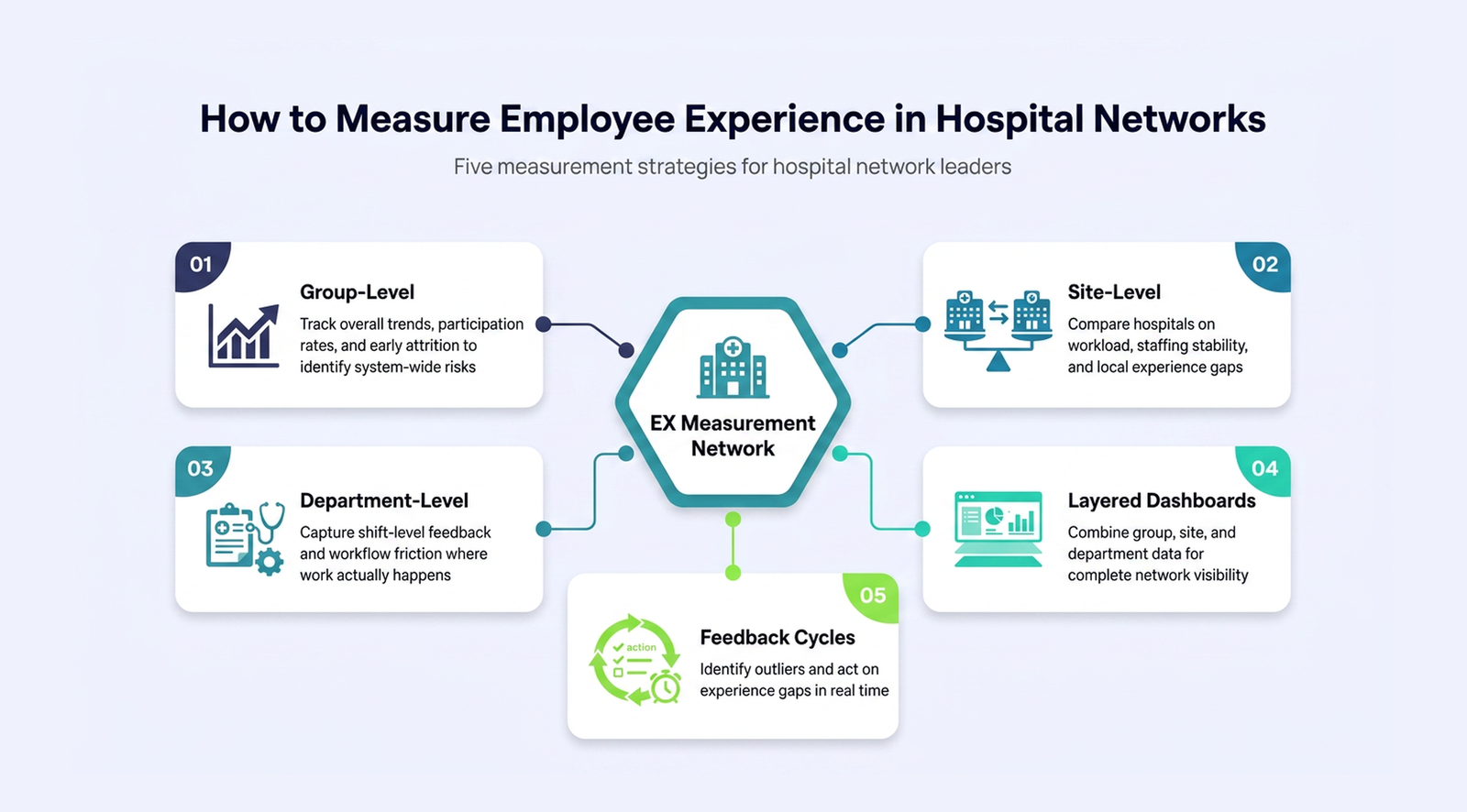
How to measure employee experience across a hospital network?

To measure employee experience across healthcare organizations, use a layered dashboard that separates group, site, and department-level metrics. Workforce experience measurement healthcare must reflect where experience is created, not just overall scores, supported by clear network EX analytics.
Group level: track system-wide patterns
Measure what affects the entire network's workplace culture, patient care and organization's mission.
- Overall experience trends, peer recognition, participation rates, and early attrition indicators.
- Cross-site comparisons and run continuous feedback surveys to identify outliers and systemic risks.
Site level: identify operational differences
Measure how experience varies between hospitals.
- Site-specific workload patterns, staffing stability, local experience gaps experience in healthcare.
- Performance differences in healthcare professionals linked to site type, size, and patient volume
Department level: detect real experience breakdowns
Measure where work actually happens.
- Shift-level feedback (including night shift staff), chief nursing officers-led team performance, and feedback patterns.
- Friction points in healthcare professionals, workflows, communication, and coordination experience in healthcare.
Measure experience at three levels: group for trends, site for variation, and department for root causes.
The way your employees feel is the way your customers will feel. And if your employees don’t feel valued, neither will your customers.
How to build an EX business case for hospital network leadership?
To build an EX business case for hospital network leadership, translate employee experience healthcare ROI into turnover savings, patient outcomes, and compliance impact. Hospital EX investment must be linked to measurable results, not survey scores.
1. Turnover cost savings
Healthcare leaders should connect experience and employee engagement improvements to reduced attrition.
- Calculate cost of replacing healthcare professionals, clinical roles, including hiring, onboarding, and productivity loss.
- Show how reduced attrition lowers workforce costs across the network, caters to employee well being and better patient outcomes..
2. Patient satisfaction correlation
Healthcare leaders should link workforce experience and employee engagement to care outcomes.
- Map experience scores to patient satisfaction and care quality indicators to reflect employee well being.
- Show how improved experience through employee engagement strategies increases patient satisfaction scores and reduces compassionate care errors.
3. Accreditation and compliance readiness
Healthcare leaders should position EX as a risk and compliance lever to improve patient outcomes and a positive employee experience.
- Demonstrate how experience design and employee engagement strategies improves documentation, communication, and protocol adherence.
- Show readiness for audits, accreditation reviews, and regulatory standards.
CultureMonkey benchmark · 2025–2026
🏥
-0.06
engagement
score drop
Healthcare engagement has declined for 3 consecutive survey cycles
Across 8 industries tracked, 6 are stable or improving.
Healthcare's three-cycle decline is one of only two industries where engagement scores have failed to stabilize or recover.
Source: CultureMonkey Benchmarks, 2025–2026 · 10M+ responses
Read the full report →What tools support employee experience strategy for hospital networks?
Hospital networks need four categories of tools to run an employee experience strategy for hospital networks at scale: feedback collection, cross-site data aggregation, role-based reporting, and action workflow management.
Feedback collection tools
- Capture experience signals at the group, site, and department level
- Cover pulse surveys, onboarding check-ins, shift-level feedback, and exit interviews
- Must support multiple channels (mobile, kiosk, email) to reach clinical staff across shifts and sites
Cross-site data aggregation platforms
- Separate data by site type, role, shift, and department, and not just overall scores
- Surface where experience breaks down at the site and department level, not just network averages
- Enable cross-site comparison to identify outlier hospitals and systemic risks
Role-based reporting dashboards
- Give central HR teams network-level views across all sites
- Give site managers access only to their own site's data
- Give department leads shift-level and team-level feedback in real time
Action workflow management tools
- Connect feedback to follow-through insights from a site debrief result in a logged intervention, not a buried report
- Track whether action was taken at the site or department level
- Close the loop between employee feedback and visible leadership response
CultureMonkey supports employee experience strategy for hospital networks with multi-channel surveys, role-based dashboards, and real-time network EX analytics, enabling leaders to measure, compare, and act across all sites from one platform.

Last reviewed: April 2026 | Based on 2024-2025 healthcare workforce data
Conclusion
Employee experience strategy for hospital networks requires system-level design. Differences across site types, roles, and workflows demand structured frameworks, clear governance, and multi-level measurement.
For employee engagement execution across complex networks, review the best healthcare workforce engagement tools designed for multi-site healthcare environments.
CultureMonkey supports employee experience strategy for hospital networks with multi-channel surveys, role-based dashboards, and real-time network EX analytics, enabling leaders to measure, compare, and act across all sites from one platform.
Book a demo with CultureMonkey.
FAQs
1. What is an employee experience strategy in healthcare?
An employee experience strategy in healthcare designs how work feels for clinical staff across the full employee lifecycle, from recruitment through exit. It covers onboarding, deployment, development, recognition, and transitions. Unlike engagement, which measures a point in time, EX designs a complete system.
2. How does employee experience differ across hospital site types?
Acute hospitals need intensity management and psychological safety. Community hospitals need continuity and belonging. Specialist centers prioritize mastery and autonomy. Aged care requires purpose alignment and staff dignity. A single EX strategy applied uniformly across all four site types consistently underperforms.
3. How do hospital networks govern EX across multiple sites?
Effective network EX governance uses a hub-and-spoke model. The central people team sets experience standards, measurement frameworks, and design principles. Individual sites customize within those parameters to fit local workforce culture, site type, and operational context, balancing consistency with relevance.
4. What metrics should hospital networks track to measure employee experience?
Hospital networks should measure employee experience at three levels: group-level trends such as participation rates and early attrition indicators, site-level metrics including staffing stability and workload patterns, and department-level data covering shift feedback and communication friction points.
5. How does employee experience affect patient care quality in hospital networks?
Stronger employee experience in hospital networks correlates directly with patient care quality. Staff who report role clarity, workload balance, and psychological safety show lower error rates, higher patient satisfaction scores, and stronger protocol adherence across clinical departments and sites.
6. How do you calculate ROI from an employee experience investment in healthcare?
Calculate healthcare EX ROI by connecting improvements to three cost drivers: turnover savings from reduced clinical attrition, patient satisfaction score changes linked to staff experience improvements, and accreditation or compliance readiness gains tied to documentation and protocol quality.
7. What is the difference between employee experience and employee engagement in healthcare?
Employee engagement measures how motivated staff feel at a point in time. Employee experience covers the full arc of how work is designed, delivered, and improved across roles, sites, and lifecycle stages. In healthcare, experience gaps persist even when engagement scores appear stable or improving.
8. What makes EX governance different in multi-site hospital systems versus single hospitals?
Multi-site hospital systems require governance that separates network-level standards from site-level customization. A single hospital applies one EX model. A network must define what stays uniform and what adapts locally, requiring clear decision rights, shared metrics, and regular cross-site performance review.













